The luxurious starter, the turkey dinner with all the trimmings, the delicious dessert, a dance round the cheese board, regular dips into the sweets jar, and if you have type 1 diabetes – stubborn high glucose levels all day!
Sound familiar?
It does to me!
I recall stubborn highs negatively impacting Christmas days because I got angry with my CGM high alert buzzing like an old fridge. Pumping loads of extra insulin, and nothing seems to happen.
It topped off with me saying.
“I am not doing this again!” – suggesting I will not overindulge on Christmas day with my friends and family, which is a sad mindset.
Over the years, I have learned how to deal with stubborn highs.
I will lay out the three approaches for consideration.
Before that.
What causes stubborn highs after eating luxurious meals high in fat?
Simple answer.
The high-fat content of the meal increases the fat delivered to the liver and muscle cells, causing the insulin not to work as well. The insulin key cannot open the cell doors as well as usual because the locks are rusty from the high fat. Less glucose leaves the blood; the glucose level goes high despite having administered the correct amount of insulin for the carbs in the meal.
The more technical explanation is that a high-fat meal increases the diacylglycerol (DAG) content in the muscle and liver cells, causing insulin resistance, as shown in the picture below (skip the image if you are happy with rusty locks).
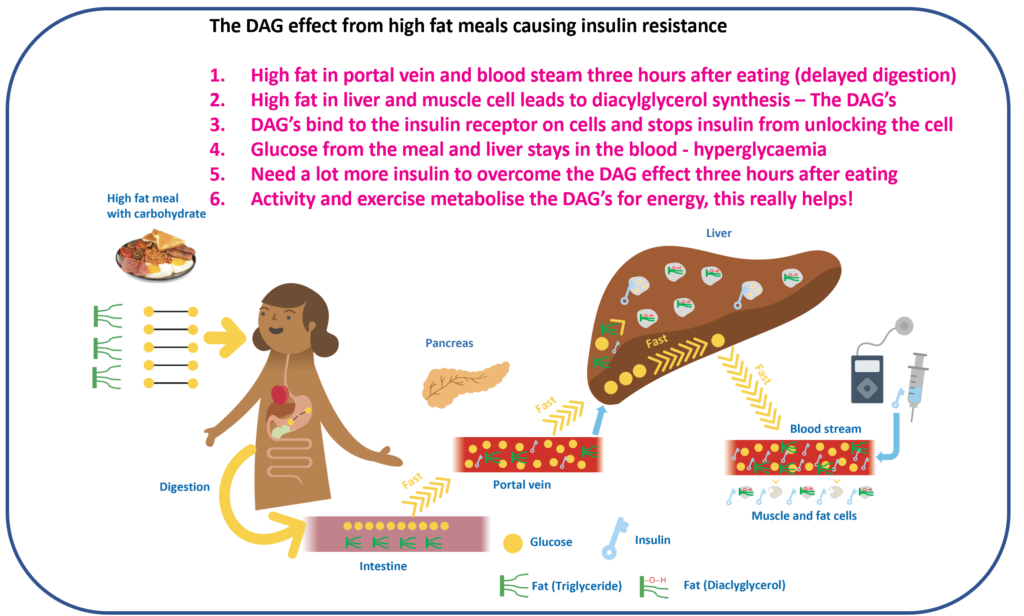
Extra insulin or more activity is needed to overcome the rusty locks.
Here are three approaches.
The blindfold approach
Having to deal with the stubborn highs on Christmas Day can consume attention and suck the festive fun out of the day. If putting in the extra effort is too much, consider the blindfold approach with safety boundaries. Of course, check with your diabetes team.
- Set the CGM low alert a little higher at 4.4mmol/L (80mg/dL) and the high alert much higher at 20.0mmol/L (360mg/dL).
- Give your usual mealtime insulin for the food consumed, and consider adding an extra 25% for the main meal.
- Consider putting a temporary basal rate increase of 25-50% extra once eating starts if using a pump.
- Keep your CGM out of sight.
- Only react with correction doses if the high alert goes off and hypo treatment for the low alert.
- Deal with the consequences on boxing day and get fully present with family.
One day of erratic glucose readings may be worth being fully present with family and friends. There is no shame in this at all. It’s about knowing yourself!
Life is much more manageable with an automated insulin delivery system, such as Control IQ, 670G, 780G, CamAPS Fx, Omnipod 5, or a DIY. The automatic increases in insulin will help.
However, the systems are designed to manage your usual sensitivity to insulin, and high-fat Christmas day meals increase insulin resistance beyond what is typical.
Here are some thoughts on how to support the systems in overcoming insulin resistance (check with your diabetes team):
- Control IQ – Set a profile for the day that makes all settings more aggressive by 20-40% and change that profile before the Christmas lunch starts.
- CamAPS FX – Set Boost working just before Christmas lunch starts.
- 670G, 780G, Omnipod 5 – dial in 25% more carbs than you eat.
- DIY – Set a more aggressive profile or use innovative settings developed by the #wearenotwaiting community.
I do not use an Automated Insulin Delivery System, and I am too much of a control freak to use the blindfold approach.
I would have less attention to the present. I like to know my glucose level.
Again, it’s about knowing yourself!
Therefore, to maximize time in range (3.9-10.0mmol/L of 70-180mg/dL), there are two main strategies.
Let’s explore them both.
The extra insulin approach
The rusty locks from the high-fat meals need extra insulin to supply brute force to open them.
How much extra?
This is the million-dollar question that has a different answer for every person with type 1 diabetes (because we are unique!)
The classic pizza study explains what I mean.
Dr. Bell took ten adults with type 1 diabetes into the laboratory to test how much insulin was needed for a 60g carb pizza base and how much extra was required for the same pizza base covered in yummy cheese and toppings.
Guess how much extra.
65% extra on average!
For example, increasing a 10-unit fast-acting mealtime insulin dose to 16.5 units.
Not only that, the insulin needed to be spread out over two and a half hours to make sure the insulin delivery matched high-fat pizzas digestion.
Did all ten people need 65% extra?
Of course not.
One person only needed 17% extra, yet, one person required 124% extra!
I said everyone with type 1 diabetes is unique.
Bottomline. Extra insulin above that needed for the carbs is unavoidable if the Christmas dinner is proper!
Here are some options to consider and check with your diabetes team:
- Whatever carbs are consumed for the meal, increase the carb value by 25-50% when calculating the insulin dose. Spread the insulin over two and a half hours on a pump or by two injections separated by at least 60 minutes.
- When correcting high glucose levels after the Christmas dinner, make the correction stronger by 25-50%
- Increase the basal rate by 25-50% as the meal starts till bedtime if using a pump
The more movement approach
Moving more keeps the glucose levels in check:
- The mealtime insulin is pumped to the muscles faster, so it works quicker.
- The kidneys break down less insulin because more insulin is pumped to the muscles for use before being cleared from the system. Therefore, being active makes mealtime insulin stronger by 25-50%, so you may not need extra if you move enough.
- Being active opens a side door to the muscle cells that do not have a rusty lock and do not need insulin to open it. The side door sucks more glucose out of the blood, so extra insulin may not be required.
- Moving reduces insulin resistance by burning up some DAG inside the muscle and liver cells.

Therefore, you could consider the following (check with your diabetes team):
- A 30-minute walk after the main course. Then enjoy the dessert. But another 30 minutes may be needed after dessert!
- Play on the new game consoles after the meal. Try a game that requires a lot of movement, such as Just Dance.
- Arrange a game of football outside after dinner. Make it competitive, younger vs. older generation, Smiths vs. Jones’s, boys vs. girls, etc.
- If Santa got presents that required movement to work them (I hope he did), now is the time. Test out the new bike or punching bag.
It may be wise to combine both extra insulin and more movement. For example, you may only require 25% more insulin if you manage a 30-minute walk after the main meal.
The beauty of extra activity is – It’s great for everyone in the family.
The person with type 1 diabetes gets to see how much extra insulin is needed and the value of movement on Christmas Day. In contrast, the person without type 1 diabetes has a pancreas that is stressed by working overtime, and insulin resistance increases glucose levels.
Get moving because it’s good for the family, not because you have type 1 diabetes.
One final note.
Be careful with hypos overnight if you plan to hit the alcohol hard.
Hypoglycemia during the day is unlikely with high-fat meals. However, if you have more than eight units of alcohol (three pints, bottle of wine, three generous home pour spirits), take precautions to prevent hypos overnight. For example:
- Set the low alert a 5.5mmoll/l (100mg/dL)
- Temporary basal rate reduction by 20%
- 20g carb snack if glucose is lower than 7.0mmol/L (126mg/dL) before bed.
Above all, enjoy the day and tackle it your way.
Related and helpful articles:
How to avoid losing control of glucose control during the holidays
