Mealtime Insulin Guide — Part 3
High-Fat Meals: How to Conquer Pizza
High-fat meals often look fine for the first hour or two — then glucose climbs later and needs much more insulin than expected. This page explores the mechanism and three practical approaches.
What counts as a high-fat meal?
These are meals where fat and carbohydrate combine to produce a delayed, prolonged glucose rise — the classic “looked sorted, then climbed” pattern.
- Examples: full English breakfast, buttery pancakes with maple syrup, thick cheese on toast, cheesy pizza, fish and chips, fast-food burger and chips, lasagne with chips and garlic bread
There are more than three ways to manage these meals. The approaches below are the ones that tend to work consistently in real-world practice — and they give a clean starting structure to experiment from.
What happens after a high-fat meal
High-fat meals often create a delayed second rise. Glucose can look stable for the first 1–2 hours, then climb later and need much more insulin than expected.
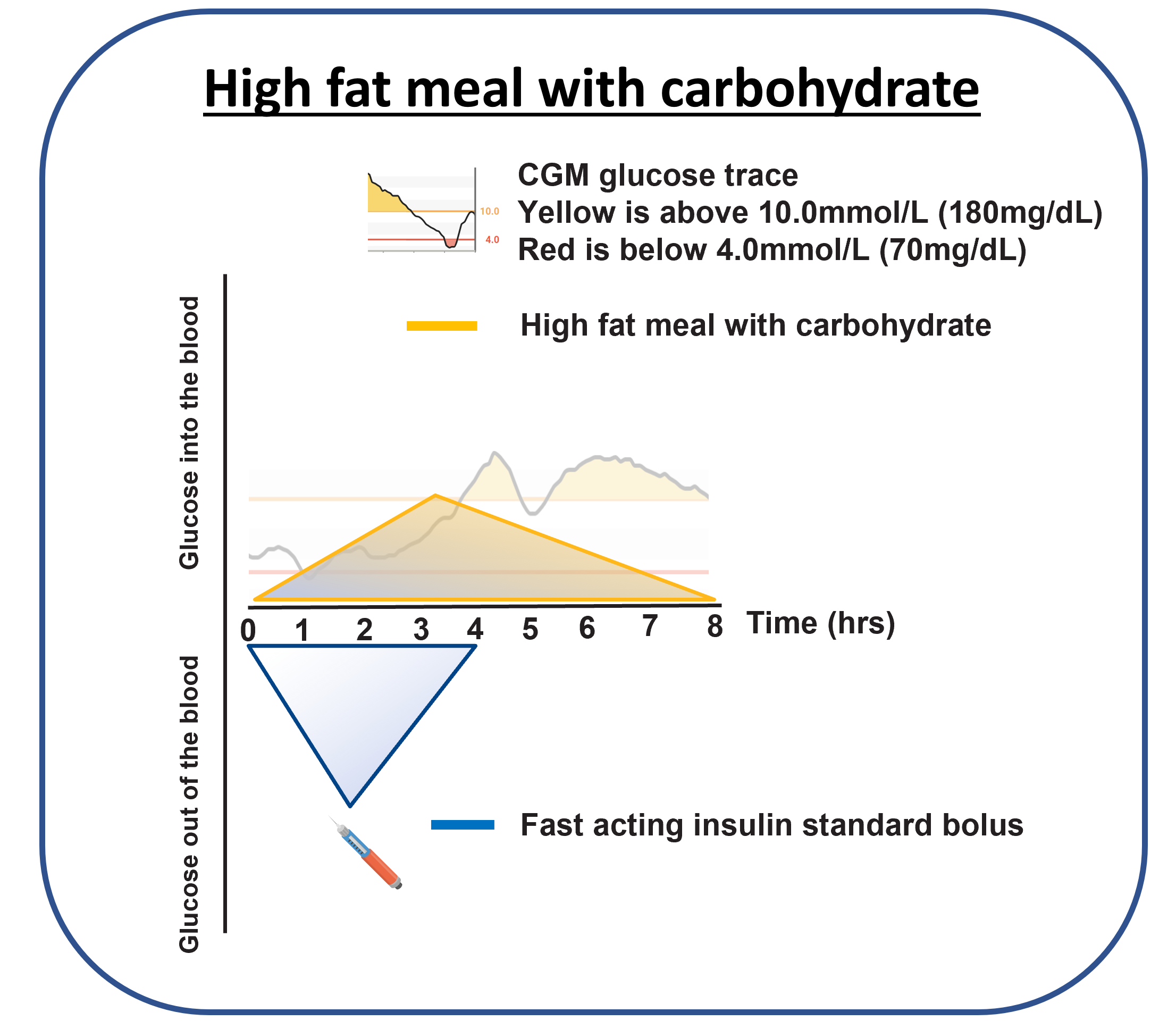
Why glucose rises hours later
Two things tend to collide:
- Delayed digestion: fat slows gastric emptying, so carbohydrate arrives in the bloodstream later than expected
- Temporary insulin resistance: after high-fat intake, intracellular lipid intermediates (diacylglycerols, or DAGs) can interfere with insulin signalling — the mechanism described by Shulman and colleagues
For a deep dive into the insulin resistance mechanism, Gerald Shulman’s work is the reference: The Drive Episode 140 — Gerald Shulman on insulin resistance.
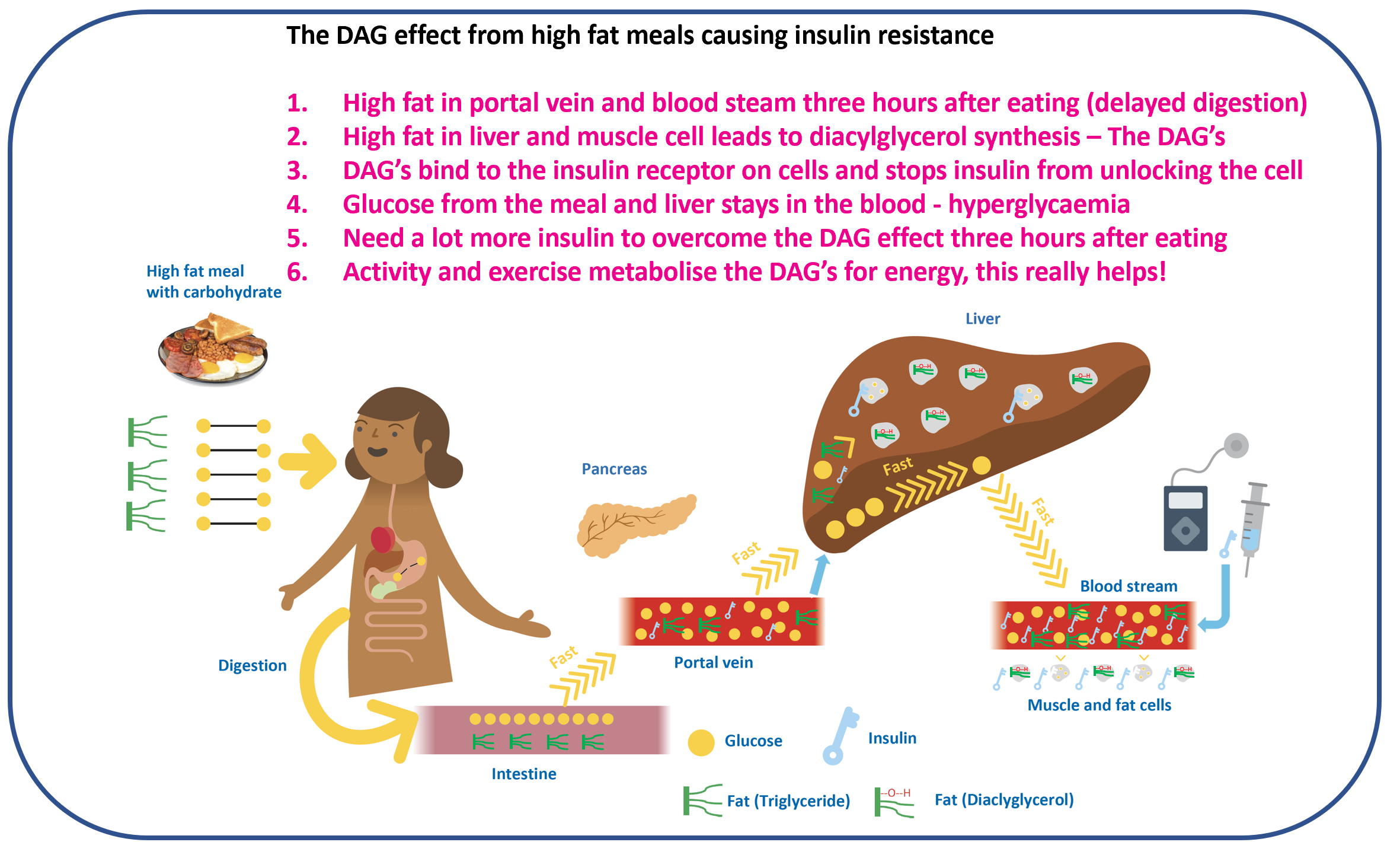
A word about insulin load
It is possible to manage high-fat meals by using a lot of extra insulin. But that often means running high insulin levels in the systemic circulation more of the time — which is not how physiology is designed to work. People without type 1 diabetes run high insulin mainly in the portal vein, not the peripheral bloodstream.
If high-fat meals become frequent, it is worth tracking the bigger picture — especially total daily dose and units per kilogram — alongside glucose metrics. The Measuring success page is a useful reality check.
Option 1 — Split and extend the insulin
This is the default approach: add extra insulin and spread it out to cover the delayed rise.
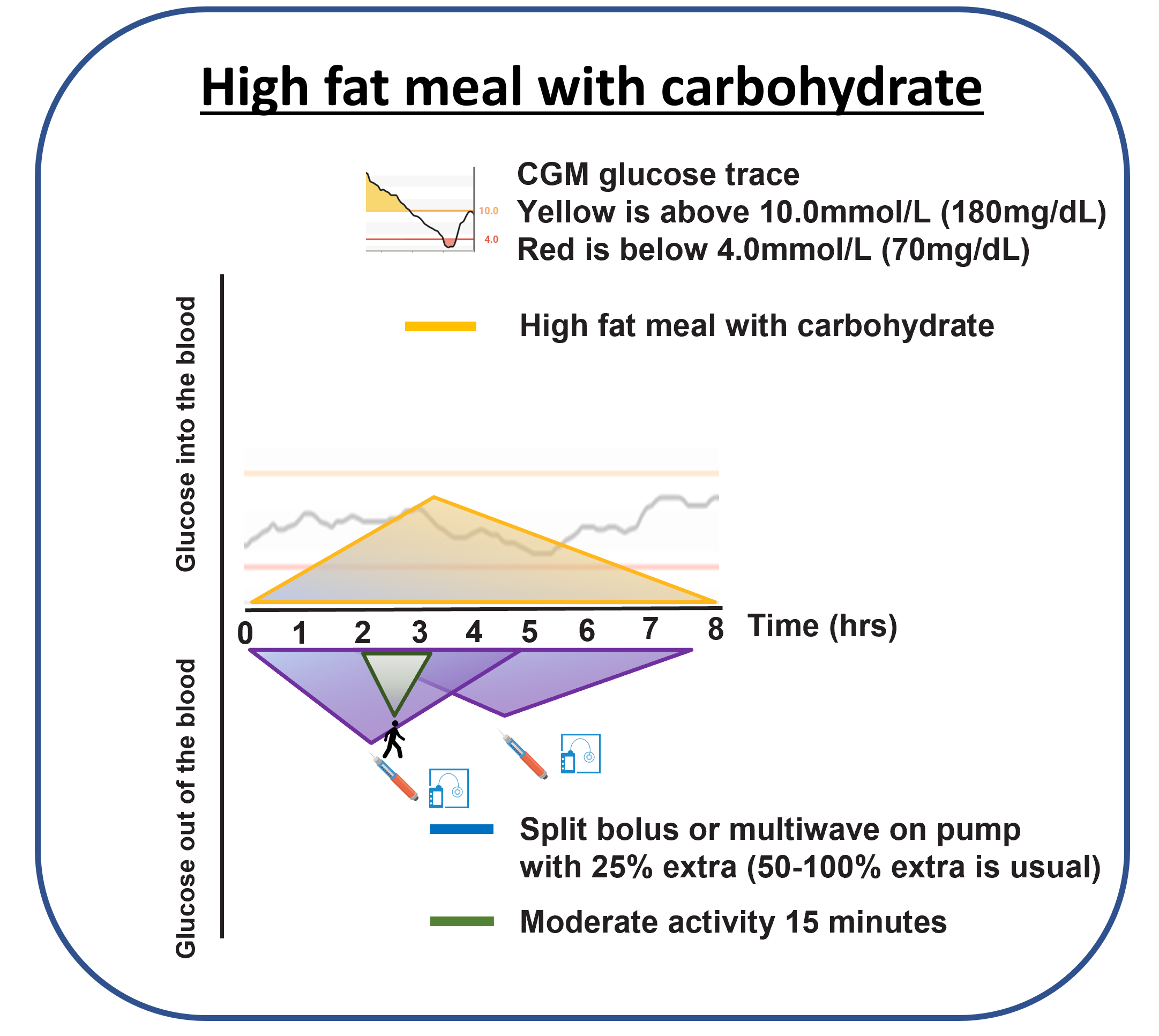
How to experiment safely
A structured way to find the right dose without guessing wildly:
- A meal only qualifies as “high-fat enough” for this approach if your CGM has already shown the delayed rise. The glucose never lies — let the data be the entry criterion
- Next time you eat that same meal:
- Count carbs and calculate the usual mealtime dose
- Increase the dose by 25% to start (dose multiplied by 1.25)
- Split the total dose roughly 50/50
- Pump: 50% up front, 50% extended over 2 hours (adjust duration based on your CGM pattern)
- Injections: 50% before the meal, 50% about 1 hour after
- If possible, add around 15 minutes of moderate activity at about 2 hours after eating
- If glucose is still high 6 hours after the meal, next time increase the extra insulin by another 25% and repeat
Many people find that high-fat meals need around 50% extra insulin on average — and some meals (pizza being the classic example) can require more.

Option 2 — Use activity as an insulin sensitiser
This option is simple but demanding: be very active after the meal. Activity does three things that help:
- Makes insulin stronger and longer-lasting
- Opens glucose uptake pathways into cells that do not require insulin
- Burns up DAG inside the cell for energy, so insulin signalling can work again
The Activity Snacking podcast explores this approach in detail.

The result of combining these mechanisms tends to look like this:
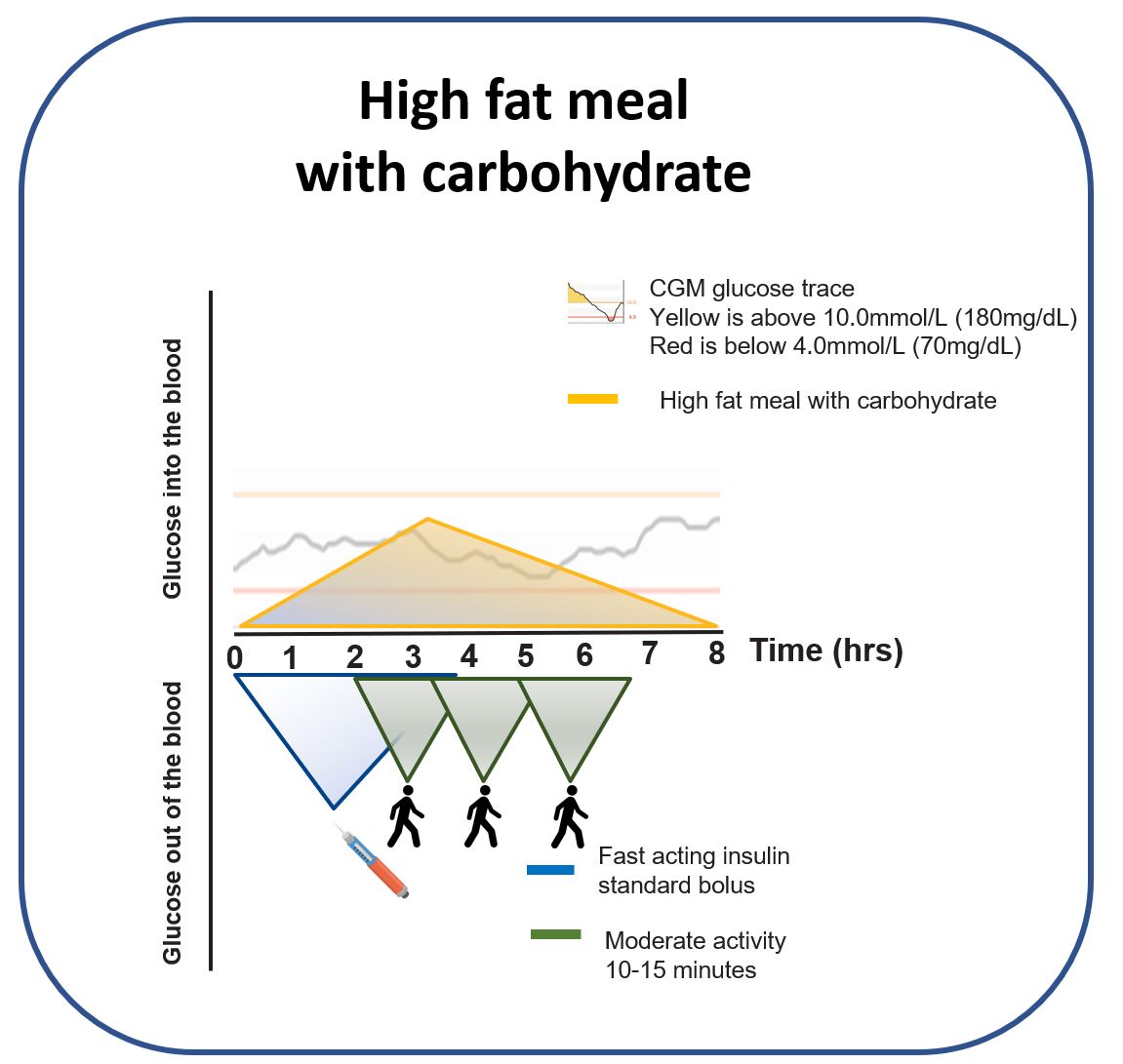
Option 3 — Accept the rise, then use GAME
If the meal is going to do what it does, a controlled response is an option: set your high alarm and use the GAME framework to stop the high without stacking repeated corrections.
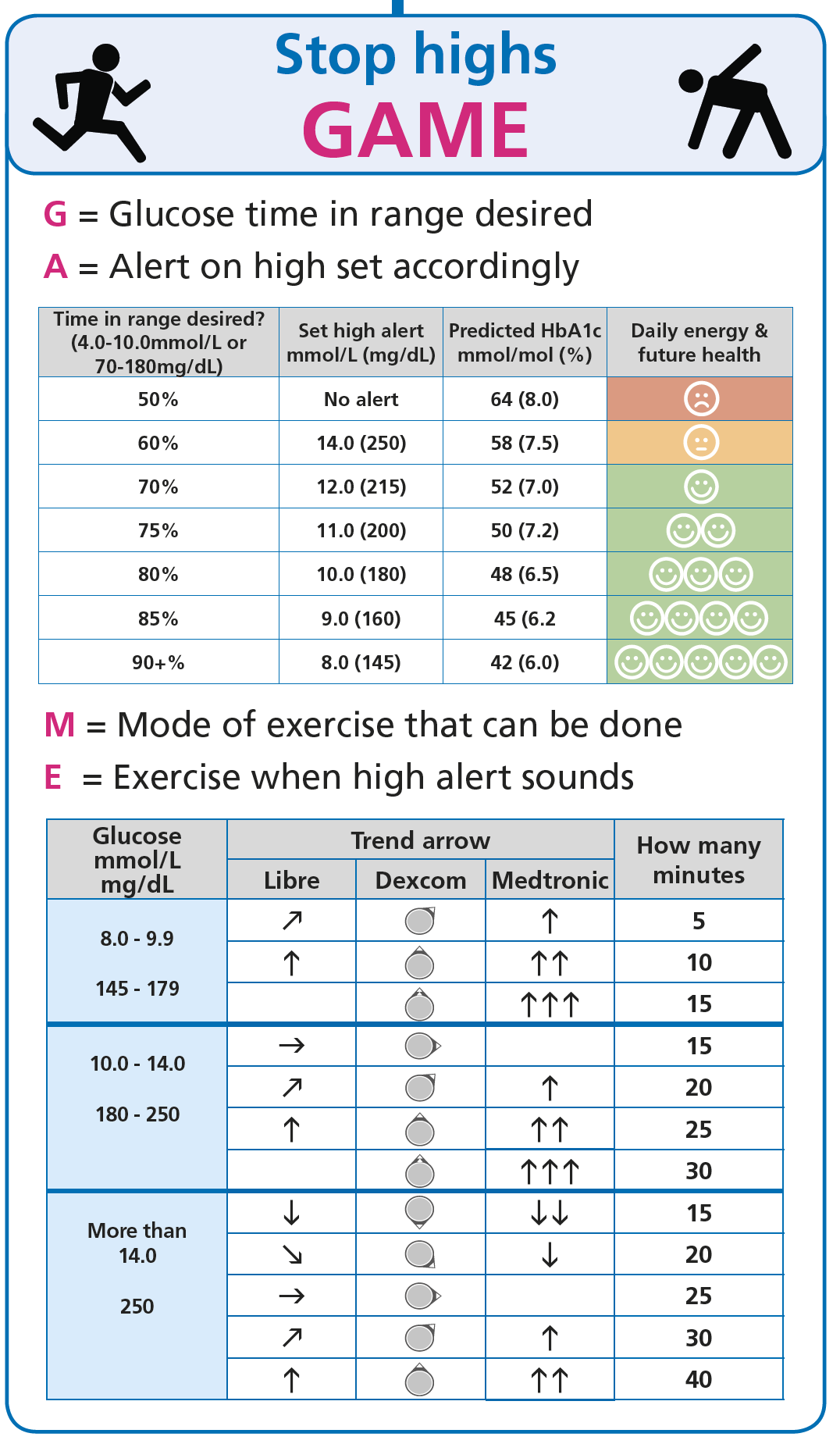
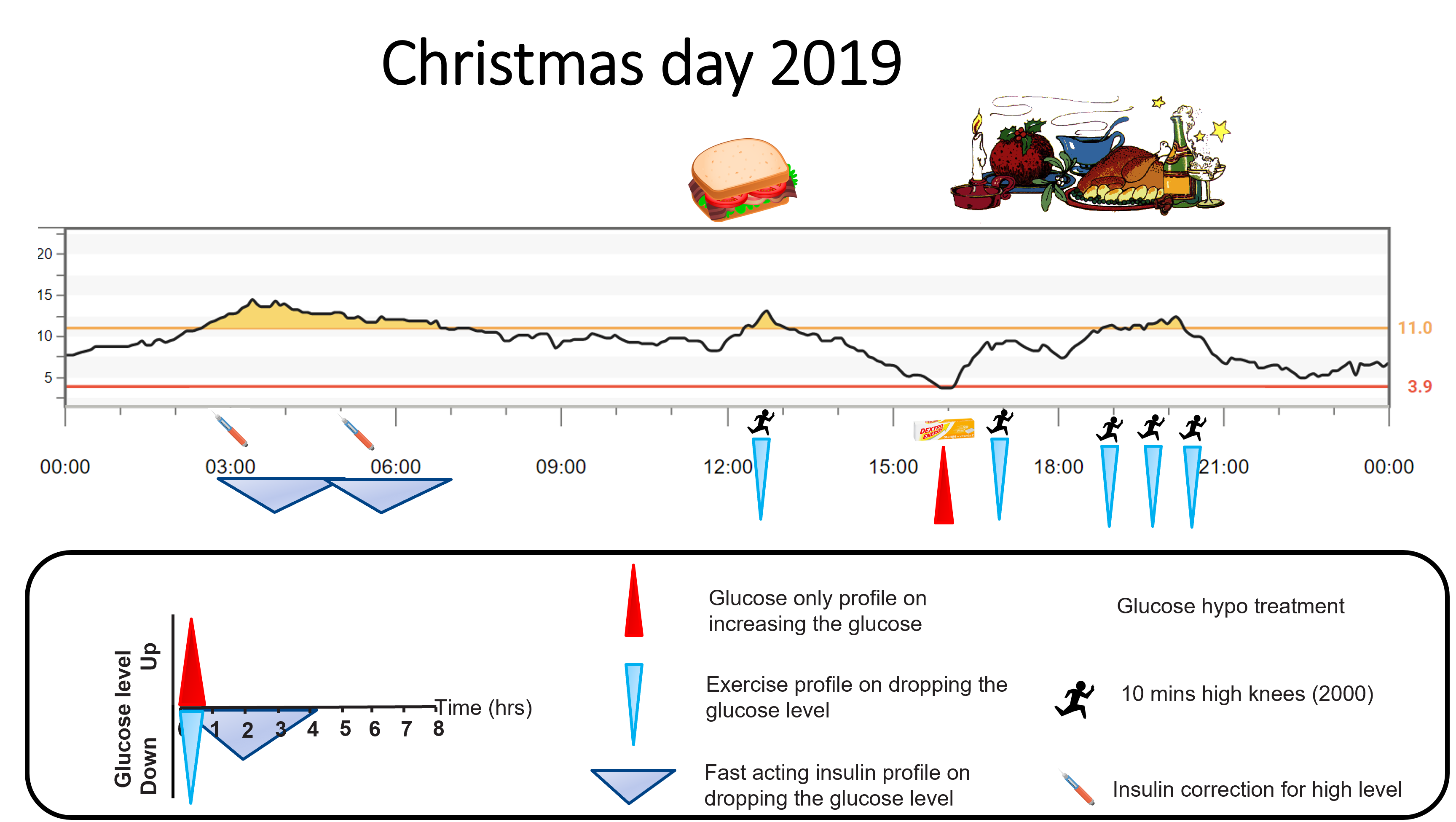
What this means in practice
- High-fat meals cause a delayed, prolonged glucose rise because fat slows digestion and temporarily reduces insulin sensitivity
- Splitting the bolus and extending it over 2 hours tends to match insulin to the delayed glucose profile
- Post-meal activity is a powerful insulin sensitiser that also clears intracellular fat intermediates
- If neither approach suits the situation, setting a high alarm and using a structured correction framework avoids correction stacking
- This is worth exploring with your own CGM data — try one approach with a meal you eat regularly and compare the 6-hour trace
This content is for educational exploration only. It describes average responses and general principles. It is not medical advice and cannot replace individual clinical guidance from your diabetes care team.

